Treat Active Acne Before Addressing Scars

Before treating acne scars, it is essential to thoroughly treat active acne first.
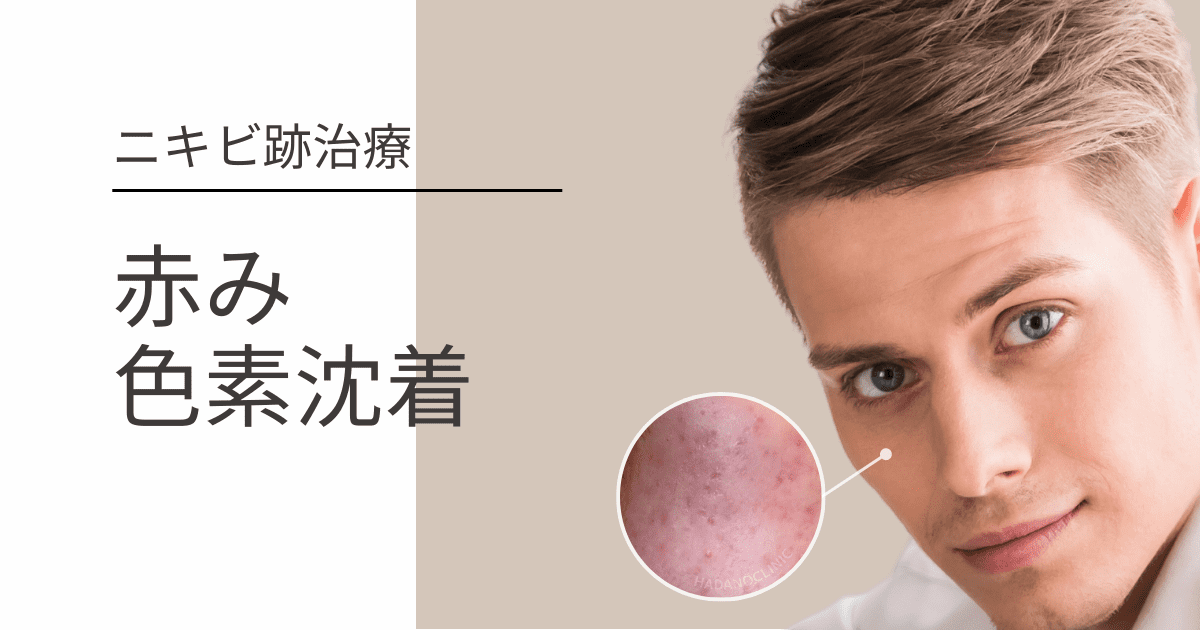
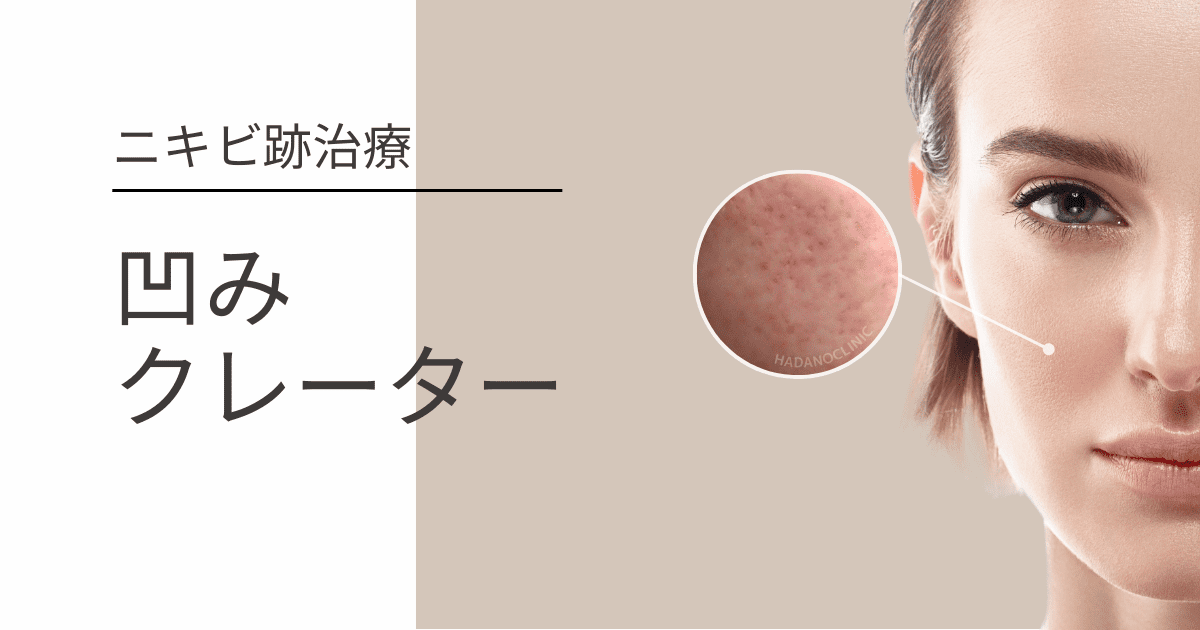
This is because acne is the root cause of scarring, including pitted scars and redness. Without addressing the underlying cause, new scars will continue to form.
In some cases, patients may have subtle acne lesions that they are unaware of, causing chronic inflammation in the skin.
During consultation, if active acne is present, our clinic will recommend comprehensive “acne treatment” alongside acne scar therapy.

HADA NO CLINIC’s Acne Scar Treatment
Hada no Clinic’s acne scar treatment is categorized into three main types based on scar characteristics. Please refer to each dedicated page for detailed information.